Health Intel AI Platform: Real-Time Diagnosis Support with AI
Health Intel AI is an enterprise-grade clinical intelligence and decision support system that combines standardized healthcare data (OMOP + FHIR), multimodal machine learning, and GPT-4 level medical reasoning.
The platform transforms fragmented patient information into real-time, evidence-based insights for diagnosis support, risk prediction, treatment optimization, and automated documentation — directly within clinical workflows.
It enables physicians, care teams, researchers, and payers to move from reactive care to proactive, data-driven intervention while maintaining full regulatory compliance.
Business Challenges or Pain Points Addressed
Massive volumes of patient data locked inside incompatible EHR systems.
Physicians spending 2+ hours daily on documentation instead of care.
Hundreds of alerts with very low clinical relevance, creating fatigue.
Difficulty correlating history, symptoms, medications, and outcomes in real time.
Static models that degrade quickly without retraining and monitoring.
Increasing pressure to improve HEDIS and quality metrics.
Rising readmissions, sepsis events, and preventable escalations.
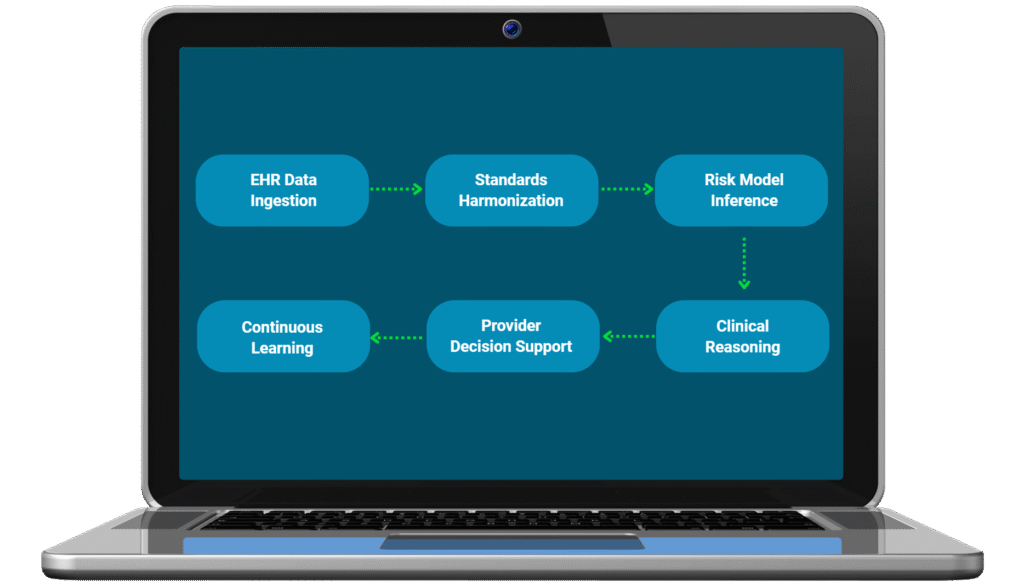
Our Solution Approach
Health Intel AI builds a unified clinical intelligence layer across structured and unstructured data, delivering actionable recommendations at the point of care.
By harmonizing OMOP CDM and FHIR standards, running ensemble ML models, and applying GPT-4 powered reasoning grounded in medical ontologies and guidelines, the system augments clinical judgment rather than replacing it.
Key pillars of the approach:
Real-time ingestion from major EHR platforms.
OMOP ↔ FHIR bidirectional mapping for interoperability.
Multimodal ML ensemble for risk, outcomes, and interaction modeling.
GPT-driven clinical reasoning referencing best-practice guidelines.
Ambient voice capture for automated documentation.
Continuous learning with drift detection and provider feedback.
Enterprise security aligned with HIPAA, GDPR, HITRUST, ONC.
Tools & Technologies Used
AI / Reasoning: Azure OpenAI GPT-4o
ML & Training: TensorFlow, Keras, Scikit-learn
Data Standards: OMOP CDM v6.0, FHIR R5
Medical Ontologies: SNOMED CT, ICD-11, LOINC, RxNorm
Backend: FastAPI, Python
Frontend: React, TypeScript
Pipelines: Apache Airflow, Dask
Security: OAuth2, HIPAA/GDPR aligned architecture
Core Features of This Solution

OMOP + FHIR Harmonization Engine
Bi-directional mapping across standardized healthcare models unifies fragmented EHR, claims, and clinical data.
Multimodal ML Ensemble
A library of specialized models predicts deterioration, readmission, drug interactions, and outcomes using structured and contextual signals.
GPT-4o Clinical Reasoning
LLM-powered interpretation converts patient context into evidence-based diagnostic and treatment recommendations.

Ambient Clinical Voice & Documentation
Automatically converts physician-patient conversations into structured EHR notes, reducing administrative overload.

Real-Time Risk Scoring
Parallel execution of dozens of clinical models delivers sub-second alerts inside existing workflows.

Federated & Continuous Learning
Models improve across institutions while preserving privacy, security, and governance requirements.
Tangible Business Value Across Functions

Physicians & Care Teams
Spend more time with patients and less on systems while receiving prioritized, explainable clinical guidance.

Hospital Operations
Reduce ICU transfers, prevent avoidable complications, and optimize resource utilization.

Quality & Compliance
Automatically identify care gaps and improve performance on HEDIS and regulatory metrics.

Population Health
Stratify risk across millions of patients to target preventive interventions earlier.

Finance & Administration
Lower readmission penalties, reduce redundant testing, and improve reimbursement outcomes.

Research & Innovation
Enable standardized, analytics-ready datasets for trials, outcomes research, and precision medicine.
Bring real-time intelligence into clinical decision making.
See how Health Intel AI augments physicians, reduces risk, and improves outcomes at scale.
Real-World Value Created Through This Automation
Up to 65% reduction in documentation burden through ambient automation.
87% precision in sepsis, deterioration, and readmission prediction.
Multi-million dollar annual savings per 100K covered lives.
Significant uplift in HEDIS and preventive care adherence.
Sub-second analytics across tens of millions of records.
High provider adoption due to workflow-embedded delivery.
What Makes This Solution Different
Unlike point AI tools, Health Intel AI is a full clinical intelligence infrastructure.
It combines interoperability, reasoning, prediction, documentation, and learning into a unified platform that works with existing EHRs rather than replacing them.
The result: explainable AI, enterprise scalability, and measurable ROI, not experimental pilots.
FAQs – Answering Common Business Asks
1. Does this replace physician decision-making?
No. The system augments clinicians with evidence-based insights, prioritization, and risk awareness while leaving final judgment to providers.
2. How does it integrate with our EHR?
Through FHIR and OMOP harmonization layers, enabling real-time data exchange with Epic, Cerner, Allscripts, and others.
3. How are recommendations validated?
Outputs are grounded in recognized ontologies and hundreds of clinical guidelines, with full traceability.
4. What about privacy and compliance?
The architecture is built for HIPAA, GDPR, HITRUST, and ONC alignment with audit trails and lineage.
5. Can models adapt to our population?
Yes. Continuous learning and federated approaches allow localization without exposing sensitive data.
6. How quickly can clinicians see value?
Organizations typically observe documentation relief and improved alert relevance within weeks of deployment.
7. Is this suitable for payers and ACOs?
Absolutely. The platform supports utilization management, high-risk identification, and quality optimization.









